Operating Room
Optimising Surgical Care with Advanced Measurements and Centralised Monitoring
Home / Operating Room
Operating Room
In today’s operating room, clinicians are faced with an increasingly complex patient population and the need to monitor these patients efficiently and effectively without increasing risk. Yet, patients are often monitored using multiple standalone devices and intermittent laboratory measurements, forcing clinicians to manually assimilate information. Masimo offers a portfolio of advanced monitoring and connectivity solutions for surgical care, including noninvasive and continuous Pulse CO-Oximetry and brain monitoring measurements, integrated into an intuitive, centralised display with automated EMR documentation.
Advanced Patient Monitoring and Connectivity Platforms
Advanced Patient Monitoring and Connectivity Platforms
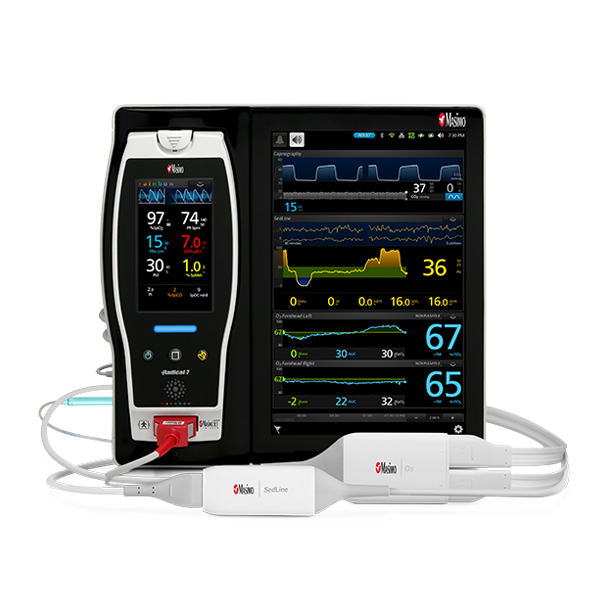
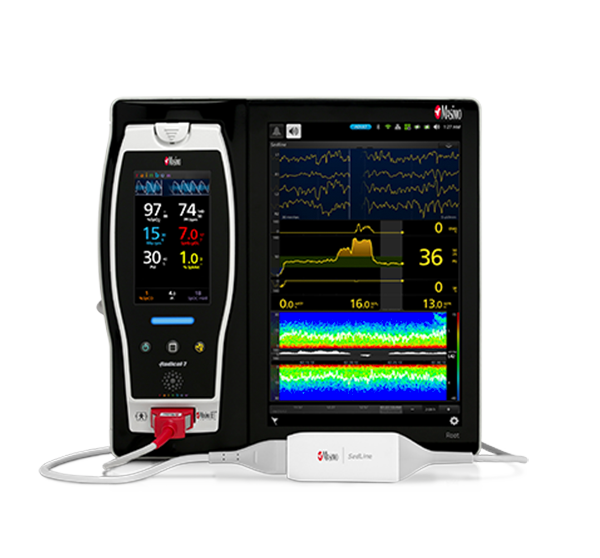
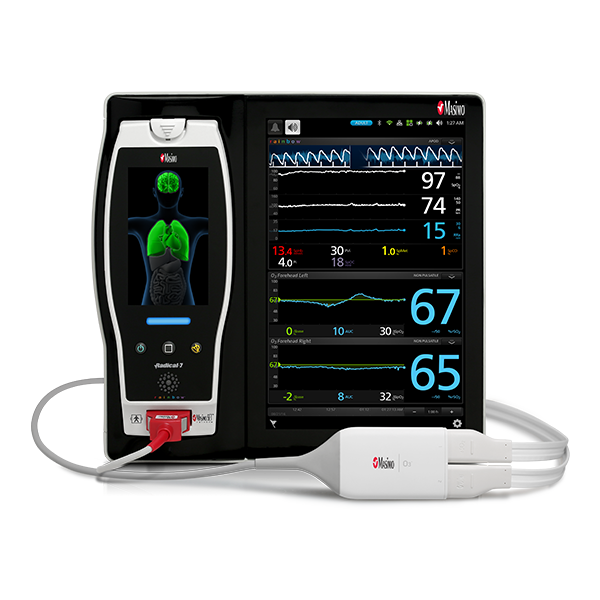
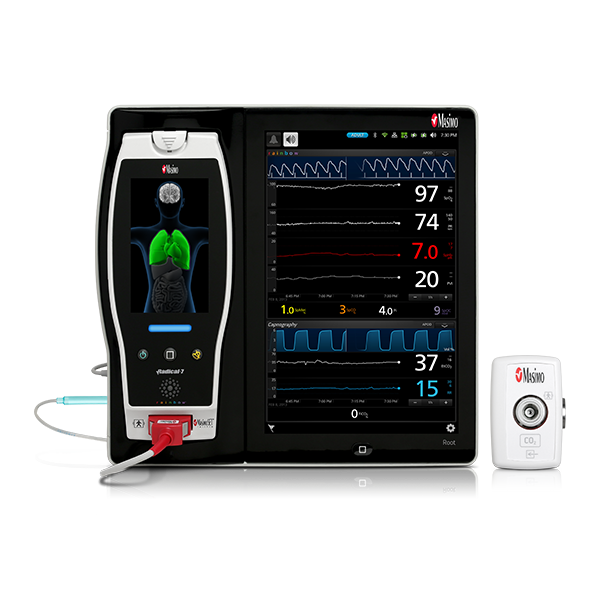
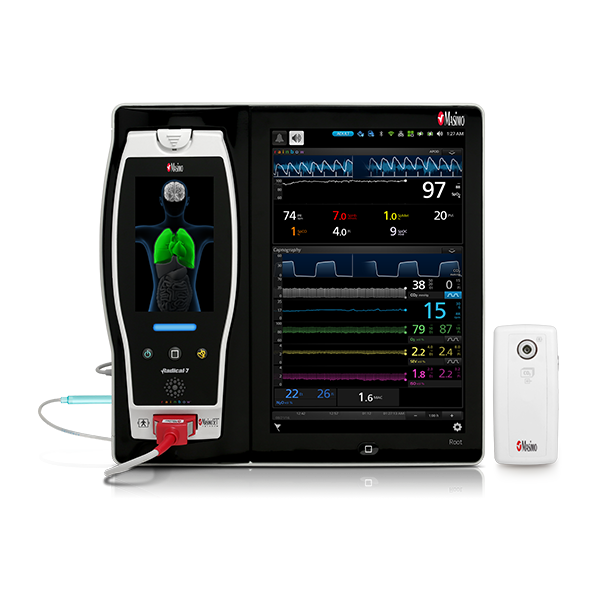
Masimo’s advanced, perioperative monitoring solutions are available together on Root®, a highly customisable, expandable patient monitoring and connectivity platform that occupies a minimal footprint in the OR. Compact yet powerful, Root provides multiple high-impact, innovative measurements on a single platform, adaptable to the patient or case, replacing many larger monitors in an area with limited real estate and empowering clinicians by providing more information in one place.
Advanced Iris® connectivity facilitates automated transfer of data from Root and multiple third-party monitors — such as IV pumps, ventilators, and anaesthesia machines – to EMRs, which may reduce the likelihood of transcription errors1 or incomplete case records.
A More Complete Picture of the Brain
A More Complete Picture of the Brain
Anaesthesia and sedation are utilised in many surgical and intensive care scenarios, but the over- and under-administration of agents is common.2,3,4 Next Generation SedLine® brain function monitoring helps clinicians monitor the state of the brain under anaesthesia with bilateral acquisition and processing of four leads of electroencephalogram (EEG) signals. Next Generation SedLine features an enhanced signal processed EEG index (PSi) with less susceptibility to EMG interference and improved performance in low power EEG cases, as well as an enhanced Multitaper Density Spectral Array (DSA).
Next Generation SedLine can be used simultaneously with O3® regional oximetry on the Root platform for a more complete picture of the brain. O3 may help clinicians monitor cerebral oxygenation of adult and paediatric patients in situations in which pulse oximetry alone may not be fully indicative of the oxygen in the brain.
Real-time Measurements
Real-time Measurements
Optimising patient blood management is an important consideration in the operating room as transfusion practices are highly variable5 and many transfusions may be inappropriate.6 However, to measure haemoglobin, clinicians are often limited to invasive blood samples, which provide intermittent and delayed laboratory results. SpHb® is a noninvasive and continuous measurement that provides real-time visibility to changes, or lack of changes, in haemoglobin between invasive blood samples.
Improper titration of fluid can lead to hypovolemia or hypervolemia that may be associated with negative outcomes.7 Pleth Variability Index (PVi®), a noninvasive dynamic parameter that helps clinicians monitor fluid responsiveness in mechanically-ventilated patients, measures the dynamic changes in Perfusion Index (Pi) that occur during the respiratory cycle. When monitored together, SpHb and PVi may provide clinicians with additional insight into a patient's status.
Preoxygenation prior to intubation can help reduce desaturations; however, inadequate preoxygenation is common.8 In addition, intubations may take longer on patients with difficult airways. Oxygen Reserve Index (ORi™) is a noninvasive and continuous parameter intended to provide insight into a patient’s oxygen status in the moderate hyperoxic range. ORi with Masimo SET® pulse oximetry can expand visibility during preoxygenation and provide potential advanced warning of impending desaturation, thereby helping clinicians intervene sooner.
Expanded Visibility
Expanded Visibility
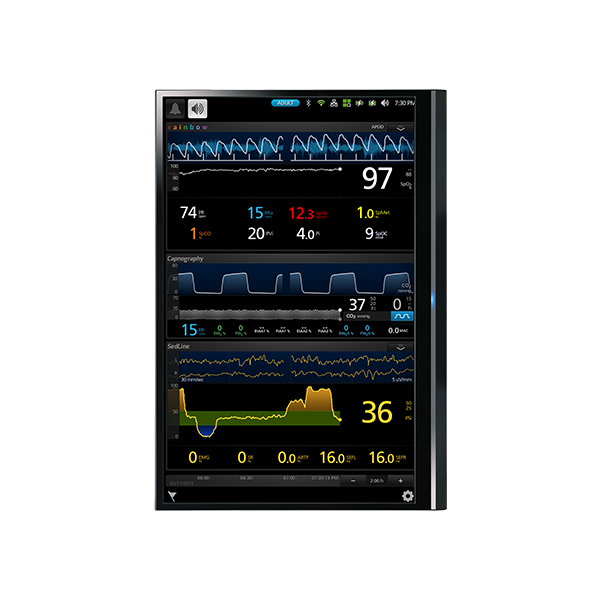
Kite® expands visibility of patient data on Root via a central, supplemental display, allowing multiple clinicians to view the same patient data simultaneously, even in a crowded environment. In addition, Kite’s customisable display allows clinicians to focus on the most pertinent data for each stage of a patient’s care, empowering clinicians to make more informed decisions.
Measurements
Measurements
Pleth Variability Index
Operating Room Solutions
References:
- 1.
The Value of Medical Device Interoperability. West Health Institute. 2013.
- 2.
Hughes, C. G. et al. Clinical Pharmacology: Advances and Applications. 2012;4:53-63.
- 3.
Jackson DL et al. Crit Care. 2009;13(6):R204.
- 4.
Simpson, Jeffrey R. et al. The American Surgeon. 79, no. 10 (2013): 1106-1110.
- 5.
Frank S et al. Anesthesiology. 2012.
- 6.
Shander A et al. TransMed Rev. 2011.
- 7.
Bellamy et al. Br J Anaesth. 2006.
RESOURCES
ORi has obtained CE Marking. Not available in the U.S. or Canada. The O3 system with paediatric indication is not licensed for sale in Canada.
Clinical decisions regarding red blood cell transfusions should be based on the clinician’s judgment considering among other factors: patient condition, continuous SpHb monitoring, and laboratory diagnostic tests using blood samples. SpHb monitoring is not intended to replace laboratory blood testing.SpHb monitoring is not intended to replace laboratory blood testing. Blood samples should be analysed by laboratory instruments prior to clinical decision making.
For professional use. See instructions for use for full prescribing information, including indications, contraindications, warnings, and precautions.
PLCO-001729/PLM-11164A-0318